Sixty-four different sites – many with high rates of child poverty and complex long-term conditions; high proportion of ethnic minorities; 14 care-commissioning groups who demand different quality metrics; and a focus on mental health and community care – not the most remunerative areas in healthcare.
All this complexity hasn’t prevented East London NHS Foundation Trust (ELFT) to set itself the audacious goal of becoming the highest quality provider by 2020!
I had the privilege of sitting in on a presentation being made by Dr Amar Shah, associate medical director for quality improvement (QI), and his team today (24th January, 2015) to a small group of Harvard Business School students and representatives from The Health Foundation, a charity that promotes quality and safety in healthcare in the UK.

“Application of QI to mental health hasn’t really been done anywhere as yet… so we have to be very innovative as many of the problems we face don’t have any readymade solutions” said Dr Shah as he started off the presentation.
He pointed out that there were no evidence–based bundles for improving mental health unlike many areas of acute care such as reducing central line infections.
Stable senior leadership, champions of quality at the top, and robust finances were some of the factors identified by Dr Shah for the Trust’s success in driving the quality agenda. He pointed out that ELFT chief executive (who has been here for 7+ years) believes in quality over money and that their medical director had come from the National Patient Safety Agency (NPSA) with deep knowledge of improving quality and safety.
Five years ago their Trust had two sentinel events – an inpatient homicide (one patient killed another) and an inpatient suicide. “This made us think… these incidents happened despite good quality assurance… we realized we had to go beyond.”
“We will have to improve quality while earning less – this isn’t possible without innovation and redesign, and eliminating waste in processes” said Dr Shah referring to the declining reimbursement for care. He also clarified that though cost is typically lowered and quality improves when waste is removed, the QI program was not about cost-cutting but improving quality!
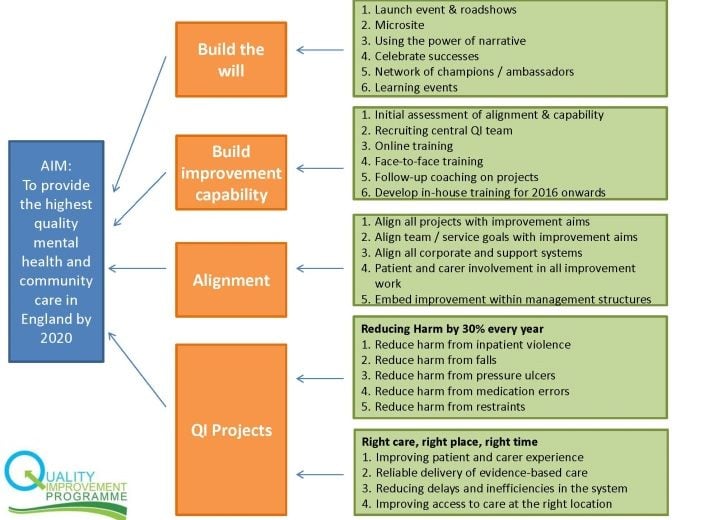
James Innes, the head of quality improvement, presented how ELFT hoped to achieve this audacious goal. ELFT has identified four drivers for achieving their aim as seen in the figure below. 
Image Courtesy: ELFT Quality Programme Presentation
I was impressed by how thoughtfully they are building the will for quality leadership through a new website and events showcasing their successes.
To build improvement capability they have partnered with the IHI to get strategic advice and run training programs for staff at all levels. For example, over 500 front-line staff will be trained in 5 six-month “waves” of training and 250 clinical leaders will be given deeper understanding of the improvement methodology.

Image Courtesy: ELFT Quality Programme Presentation
The ELFT team is working to ensure alignment so that projects are focused on two stretch goals:
- Reduce harm by 30% every year, and
- Provide the right care, at the right place, and at the right time.
And in less than a year they already have 114+ projects going!
Dr Genevieve Holt, a QI Clinical Fellow who recently completed the prestigious Darzi Fellowship in clinical leadership, discussed an example where the Trust targeted a reduction in weight gain for patients who were hospitalized.
She shared her insight of how it was important for the team to come together to generate change ideas in order to have ownership for the project and how improvement often has to begin at the very beginning – in this case, setting standards for how patients will be weighed and how this data will be captured to enable analysis.
Tsana Rawson, another QI Clinical Fellow, related how ELFT was creating an evidence base for reducing violence on mental health wards using better communication (speaking with patients uncovered that one source of tension was a tussle over what channel would be played on TV), flattened hierarchy (often lower down staff could identify patients who were at risk of becoming violent but didn’t feel comfortable speaking up), transparency and stakeholder involvement.
She shared how ELFT was using a collaborative model wherein different adult wards working on the same problem were learning from each other and accelerating improvement.

In the afternoon, I also had the privilege of joining a weekly review meeting of the QI team. I saw how Tim Gill, Programme Manager, efficiently updated progress on the various tasks while the meeting was on and learnt how Forid Alam, QI Data Analyst, was creating dashboards to increase transparency and help answer the all important question of “whether all this effort was really making a difference”!

Throughout this amazing morning, I was struck by the similarities with the journey in our own small nonprofit hospital in India. We too have turned to the IHI for guidance – our head of quality is an Improvement Advisor, a number of consultants have completed the IHI Open School Basic Certificate, and we participate in a collaborative for improving perinatal care.
We pursued quality as a fundamental aspect of our nonprofit mission and are embracing transparency, such as disclosing our caesarean section rates, without any external triggers. Even our payers don’t fully appreciate what we are trying to do and we too have to look overseas for learning!
Like ELFT, even in our case it was patient safety incidents that moved me and individual consultants to deeply reflect and commit to going down “a road less travelled”. But unlike ELFT, we have had to sustain this journey despite financial instability – quality is our strategy for winning trust and achieving financial health!
I left East London feeling inspired and uplifted – by the excellence of the work that I had seen but even more because of the humility, helpfulness and willingness of the entire ELFT QI team to share their experience. I learnt that in March they were hosting an associate medical director from a mental health hospital in Uganda that this Trust has an ongoing relationship with! I too was invited to come back or send colleagues and offered copies of their reports.
“We’re only beginning” is what Dr Amar Shah and his colleagues kept repeating as I expressed my awe and appreciation for what I was seeing. “You guys are creating magic and the world will learn from you” was my response!