In a transvaginal scan at 20 weeks, Richa Bishnoi was informed that she would have to undergo a cesarean section because her cervical length was 20 mm. Having had a miscarriage before and determined to avoid surgery, she decided to get a second opinion.
During the course of her research on hospitals and gynecologists that encouraged normal delivery, she came across the profile of Dr Namrita Gurpal Singh Sandhu, Consultant Obstetrician-Gynecologist. She scheduled an appointment without any delay.
Richa anxiously told the doctor her situation and asked for guidance.
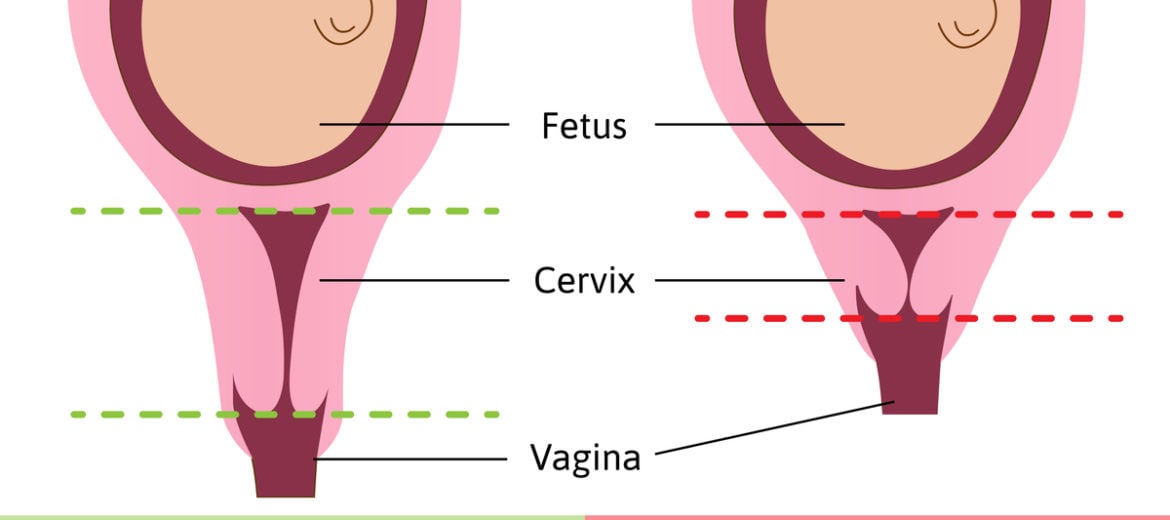
The doctor listened to her concerns and then explained “The cervix which is the mouth of the uterus is usually closed and firm in women who are not pregnant. During pregnancy, it becomes less firm and decreases in length with time. “
Richa wanted to know why the length of the cervix was measured.
Reason for Assessing Cervical Length
Studies show that the length of the cervix is an indicator of preterm births. The lower part of the uterus is not fully formed before 16 weeks and so the cervical length is measured between 16 to 24 weeks of gestation.
How is cervical length measured?
The most accurate way to measure the cervical length is through a transvaginal ultrasound. The cervical length may be measured through a transabdominal ultrasound but a full bladder may interfere with these measurements and cause the length to appear longer.
Is the Cervical Length Measured for Every Pregnant Woman?
No. Your gynecologist may advise a transvaginal ultrasound to gauge the length of the cervix if you are carrying one baby and have a history of preterm birth or miscarriage.
According to The Society for Maternal – Fetal Medicine, routine transvaginal cervical length screening should not be performed for women with cervical cerclage, multiple gestation, preterm premature rupture of membranes or placenta previa.
Richa was curious to know more about the cervical length and its implications.
Located in Delhi and looking for an experienced gynaecologist? Book a consultation with the best gynaecologists in Delhi who work together as a team at Sitaram Bhartia Hospital, South Delhi. Click the button below to book a paid consultation with us.
What is the normal cervical length?
At 20 weeks the normal cervical length is around 30-40 mm.
Women often search for a cervical length chart in mm that includes the normal cervical length at 7 weeks, normal cervical length at 30 weeks etc but actually the only measurement to go by is the normal cervical length.
What is a short cervical length?
A cervix that is less than 25 mm is considered a short cervix.
The shorter the cervix early in pregnancy, the higher the chances of a preterm birth.
Richa realized that the length of her cervix was less than the normal length and put her at risk of having a premature baby.
She asked about the causes of a short cervix.
What causes a short cervix?
Cervical insufficiency or cervical incompetence may cause the cervix to shorten and open by the second trimester. This happens because the cervical muscles may have weakened due to surgery in the cervix, a previous difficult birth or structural abnormalities in the uterus.
“So how does a short cervix cause a preterm birth?” she asked.
“The cervical length usually shortens between 28 to 30 weeks, “ explains the doctor, “during labour, when you are ready to give birth and your baby has fully developed, the cervix begins to dilate or open (termed cervical effacement) so that the baby can slide into the birth canal for delivery.”
“But if the cervix is shortened much before time, a preterm birth or miscarriage may occur.”
Richa’s forehead creased with worry.
The doctor was quick to notice and comforted her, “Don’t worry. We can treat a short cervix to help prevent a preterm delivery.”
How to Treat a Short Cervix
A few options to manage a short cervix are:
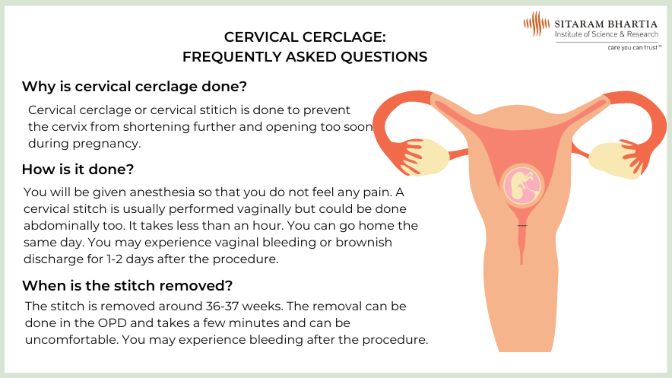
Cervical Cerclage
This is a procedure in which the cervix is stitched up to prevent it from shortening and opening further.
A cervical stitch may not be suitable for women who are experiencing contractions (because these will prevent the stitch from staying in place), vaginal bleeding or infection. Cervical cerclage may not prevent preterm labour in women with multiple babies.
Hormonal treatment through Progesterone Injections
For women with a short cervix and a history of preterm births, progesterone injections or gel application may be advised if you are carrying a single baby. The hormone progesterone helps the uterus grow and can stop contractions. This enables the pregnancy to progress to full-term (39-40 weeks and six days).
Cervical Pessaries
A pessary or silicone ring can be placed through the vagina to support the shortened cervix in women with a single baby. While cervical pessaries are used around the world, more research is needed to prove that pessaries help prevent preterm births.
After having understood all the options, Richa decided to go ahead with the cervical cerclage.
She decided to continue her consultations, considering how calmly and clearly the doctor informed her of the condition.
In her 37th week, the doctor removed the cervical stitch.
Richa then asked “ What is the ideal cervical length at 37 weeks for normal delivery?”
Is there an appropriate cervix length for normal delivery?
The cervical length should not restrict you from having a normal delivery.
“In women with a short cervix, our primary goal is to protect the baby and the mother by reducing the risk of a preterm delivery as the baby is not fully developed.”
“If a woman goes into labour prematurely, she can still have a vaginal birth. A cesarean is required only if there are complications or the baby is unable to move down the birth canal.”
Richa was relieved to hear that she would be able to try for a vaginal delivery.
Richa Bishnoi’s Birth Story
A few weeks later Richa experienced labour pains and rushed to the hospital. With her husband constantly by her side, she was able to endure labour and eventually gave birth to a beautiful baby girl.
“I was screaming and shouting but the nurses, doctor and my husband comforted and motivated me. They gave me the confidence to go through the vaginal birth I always wanted,” said Richa, caressing the baby in her arms.
Would you like to consult us about your pregnancy? Please click the button below to schedule an appointment with Dr Namrita at our hospital Sitaram Bhartia Institute of Science and Research, Delhi.
More Resources: