Sonali Bhasin, 27, squealed and jumped in joy when she saw two pink lines on her pregnancy test. After months of trying to conceive, she was finally pregnant. Or was she? Shreds of doubt creeped into her mind and she decided to consult her gynecologist.
“Based on Sonali’s last period and her positive pregnancy test, we recommended a blood test to confirm her pregnancy,” says Dr. Anita Sabherwal Anand, Consultant Obstetrician- Gynecologist at Sitaram Bhartia Hospital.
What tests are done during the first trimester of pregnancy?
All expecting women are recommended either a urine test or a blood test to confirm the pregnancy. Both tests are used to detect the presence of the Human Chorionic Gonadotropin (hCG) hormone, which is produced by the placenta.
A urine test may be done a week or two after the missed period while a blood test can be done sooner.
After the pregnancy is confirmed, you will be asked to do blood tests to check for
- Blood group
- Anemia and Thalassemia
- Thyroid dysfunction
- Diabetes
- Urine infections
- Viral infections such as Rubella, HIV, Hepatitis B, Hepatitis C and Syphilis
As your pregnancy progresses, you will be advised a first trimester screening, also known as a Nuchal Translucency (NT) scan and double marker test.
When the blood test confirmed that Sonali was indeed pregnant, her doctor informed her of the first trimester tests and screening to be done.
What does the first trimester screening test?
The first trimester screening helps assess your baby’s risk of having Down’s Syndrome (Trisomy 21) or Edward’s Syndrome (Trisomy 18).
We all have 46 pairs of chromosomes in our cells in the body. Trisomy refers to the presence of an extra chromosome in addition to the usual pair, either an extra chromosome number 21 in Down’s Syndrome or an extra chromosome number 18 in Edward’s syndrome.
Children with Down’s Syndrome have physical and mental developmental delays and children with Edward’s Syndrome have severe development issues and may not live beyond their first birthday.
“Also known as a ‘Combined test’ in some countries, this screening is offered to all pregnant women. Studies have shown that babies born to mothers 35 years and above are usually at a higher risk of having chromosomal abnormalities,“ explains Dr. Anita.
The first trimester screening includes:
- Blood tests, called double markers, which measure the blood levels of two hormones, the Pregnancy Associated Plasma Protein (PAPP-A) and the Human Chorionic Gonadotropin (hCG), which are produced in all pregnant mothers.
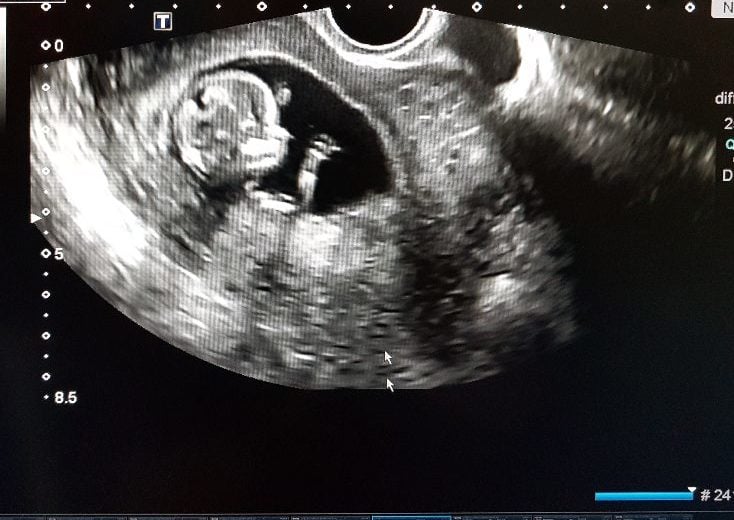
- A specialized ultrasound, called the NT NB scan or Level I ultrasound. For Down’s syndrome screening, the ultrasonologist will assess the back of the baby’s neck, and measure the thickness of what is called the nuchal fold. This measurement is termed as Nuchal Translucency (NT). Studies have shown that babies with an increased amount of fluid or nuchal fold thickness (NT) above 3mm are at higher risk of having a chromosomal abnormality.
The ultrasound is also useful in dating the pregnancy and evaluating the fetus for structural defects particularly of the skull, brain and spine.
Related: How an Anomaly Scan Helps and Why You Need It
The American College of Obstetricians and Gynecologists (ACOG) and the Royal College of Obstetricians and Gynecologists (RCOG) both recommend and offer the NT scan and double marker test so that all pregnant women are aware of the risk of these conditions early on in the pregnancy and can make informed decisions about it.
“It’s also important to realize that these tests only determine the risk of having a chromosomal abnormality and not whether your baby actually has either of these conditions.”
The first trimester screening of Down’s Syndrome and Trisomy 18 is not entirely accurate as it can identify 85% of expecting women who may have a baby with either Down’s Syndrome or Edward’s Syndrome.
Sonali had heard about these conditions but the thought of her own baby suffering from them was unfathomable. The doctor understood her concerns, counselled her and asked her to maintain a positive frame of mind.
When is the first trimester screening usually recommended?
It is advised between week 11 to 13 and 6 days, although the best time is 12 to 13 weeks.
Sonali was relieved to know that the NT scan and double marker did not require any kind of preparation. She could eat and drink normally before the tests. She scheduled her screening immediately after her consultation.
What should you expect on the day of the first trimester screening?
You will be asked to visit the laboratory at the hospital for your blood test.
“This is done like any other blood test, where a needle is inserted into your arm and blood is drawn.”
After your blood sample has been taken, you can proceed to get an ultrasound done. “Our expert ultrasonologist will apply gel over your abdomen and place a probe over it. As the probe is moved over your belly, images will appear on the monitor, allowing her to examine the baby.”
Sonali had been optimistic throughout her first trimester but when the day of her tests dawned, she was a nervous wreck.
Her husband held her hand all through the tests.
When she got the results of her first trimester screening, she nearly rushed to her gynecologist to understand what they meant.
How do you interpret the results of the first trimester screening?
The first trimester screening results range from low-risk, moderate-risk to high-risk.
- First trimester screening negative means the same as low-risk, which indicates a low chance of chromosomal abnormalities in your baby.
With a low-risk result, there are very slim chances that the baby may have abnormalities but you should understand that 1 in 10 will be missed.
“Also remember that the NT scan and double marker screen only a few conditions and are not inclusive of other problems that may be present.”
- First trimester screen positive indicates a moderate or high risk, wherein there are greater chances of your baby having a chromosomal abnormality.
In such a situation, your test results are discussed in detail and your doctor may refer you to a fetal medicine specialist. You may be recommended further diagnostic tests to determine whether your baby truly has the suspected chromosomal anomaly. These include:
- Chorionic Villus Sampling (CVS) wherein a sample of the placenta is taken and examined. It is usually done in the first trimester itself.
- Amniocentesis, wherein a sample of the amniotic fluid is removed and tested, and may be done in the second trimester.
- Cell-free DNA (cfDNA) in which the baby’s DNA is evaluated from the mother’s blood for information on any chromosomal abnormality.
Much to her relief, Sonali’s first trimester screening results fell in the normal range. Neither her family history nor her age made it necessary to test further. She sailed through the rest of her pregnancy and went on to give birth to a healthy, charming little girl.
Conclusion
Women who miss the first trimester screening or are unable to get clear results because the baby’s position makes it difficult to assess the amount of fluid at the nuchal fold will be recommended the quadruple test for Down’s Syndrome.
This is a blood test that assesses the possibility of Down’s Syndrome by checking the levels of four substances present in all pregnant mothers. These are Alpha-fetoprotein (AFP), Human chorionic gonadotropin (HCG), Estriol, and Inhibin A. It is usually done in the second trimester, at 15 to 20 weeks pregnancy.
A positive quadruple test for Down’s Syndrome points toward a higher risk of chromosomal abnormalities in your baby. Your doctor will suggest appropriate tests that may be able to confirm the presence of these genetic conditions.
“It can be unnerving to find out that your baby has a higher chance of developing a chromosomal abnormality. Couples need to understand that if all tests point towards an abnormality in the baby, there are two choices to make.
One is to undergo a medical termination of pregnancy (MTP) as the family may not be able to bear the emotional, social and financial implications of having such a child. The second choice is to continue the pregnancy and create systems appropriate for treatment and therapy of the child. We respect the choice of every couple regardless of the decisions they make,“ emphasizes Dr. Anita.
“In our experience, however, we have seen couples give birth to babies with Down Syndrome, who despite the challenges, fill their parents’ lives with a joy like no other.”
Medically Reviewed by Dr. Anita Sabherwal Anand, MBBS, MD, DNB
You May Like to Read: